What is a transsphenoidal removal for a pituitary tumour?
Transphenoidal is performed to remove a pituitary tumour from the pituitary gland. The tumour is reached by working through the nose. To accurately localise your tumour, a computerised guidance system and a microscope or endoscope is used to assist with the surgery.
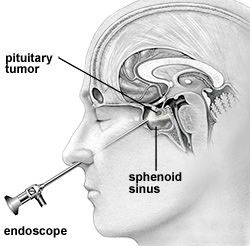
By working through the nostrils, a hole is made at the back of the nose into the sphenoid sinus, through a layer of bone between the sphenoid sinus and the pituitary gland to gain access to the tumour. As much tumour will be removed as is safe to do so.
At the end of the transphenoidal surgery, to help fill the hole from where the tumour was removed, it may be necessary to fill the hole with small pieces of fat and other tissue. These are harvested through a small cut in your thigh or abdomen. Tissue glue may be used to secure the tissue fat and other tissue in place. This helps to prevent leakage of brain (cerebrospinal) fluid.
The cut in your thigh will be closed with sutures and the nose maybe packed with a spongy material. After the procedure, you will be able to carefully wipe your nose but not blow it as air may be pushed into the brain. You will not be able to blow your nose for 6 weeks after the procedure.
What are the risks of Transphenoidal?
There are risks and complications with this procedure. They include but are not limited to the following, Infection, requiring antibiotics and further treatment. Minor pain, bruising and/or infection from IV cannula site. This may require treatment with antibiotics. Bleeding is more common if you have been taking blood thinning drugs. Pituitary dysfunction requiring further medical treatment. This may be temporary or permanent.
Some uncommon risks include heart attack due to the strain on the heart. Stroke or stroke like complications may occur causing neurological deficits such as weakness in the face, arms and legs. This could be temporary or permanent. Visual damage, this could include double vision, a droopy eye/s or blindness. This may be present prior to surgery and may not improve or may even get worse following surgery.
Meningitis may occur requiring further treatment and antibiotics. Small areas of the lung may collapse, increasing the risk of chest infection. This may need antibiotics and physiotherapy
Death because of this procedure is very rare.
